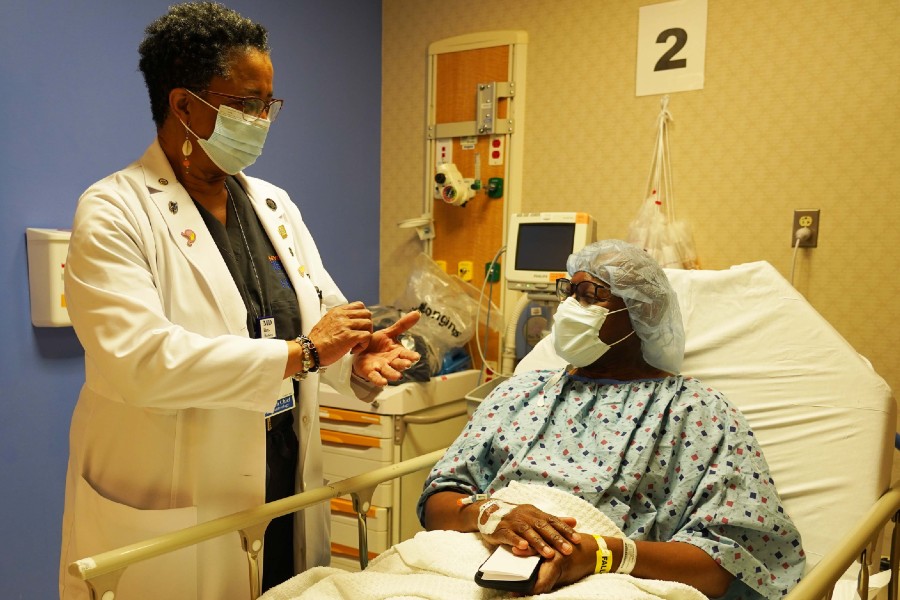
NYC Health + Hospitals today announced the success of its telehealth expansion in response to COVID-19.
NYC Health + Hospitals today announced the success of its telehealth expansion in response to COVID-19.
Within a week of documented community spread of the virus in NYC, converted all routine face-to-face visits to televisits, or scheduled telephonic visits. The City’s public health system was able to quickly scale up its telemedicine services, going from just 500 billable virtual visits in the month prior to the COVID-19 pandemic, up to nearly 57,000 in the first three weeks of the pandemic, and over 235,000 televisits to-date.
Additionally, the health system handled approximately 13,000 patient messages over six weeks during the pandemic via its patient portal, which allows patients to directly communicate with their care teams.
Additionally, the health system handled approximately 13,000 patient messages over six weeks during the pandemic via its patient portal, which allows patients to directly communicate with their care teams. Prior work under the public health system’s transformation strategy, including laying telehealth groundwork starting in 2017 and transitioning to a unified electronic medical record system, led to the rapid and successful expansion of telemedicine.
“Our priority during the unprecedented COVID-19 pandemic was to ensure that the City’s public healthcare system continued to provide New Yorkers the care they needed where it was safest – at home,” said NYC Health + Hospitals Senior Vice President for Ambulatory Care Ted Long, MD. “We were fortunate to already have a strong foundation to quickly scale up and expand these telehealth services, including other necessary services we provide our diverse patient bases, such as financial counseling and coordinated care. NYC Health + Hospitals provide patients a one-stop-shop to live their healthiest lives, and this pandemic proved our commitment.”
Other areas of patient care and support that were successfully transitioned to virtual interactions included:
- COVID-19 Hotline: NYC Health + Hospitals developed the clinical arm to NYC’s newly created 311 informational hotline dedicated to COVID-19 inquiries. Calls were routed to clinicians to screen patients for COVID-19, triage requests for COVID-19 testing, or direct patients to necessary medical care. Starting in mid-March, the system’s call volume grew from just over 1,000 calls per day to a peak volume of over 7,000 calls a day. By answering over 75,000 calls in the first month of the COVID-19 pandemic, the hotline providers helped avoid a large number of non-urgent ED visits at a time when it mattered most.
- Electronic Specialty Referrals: The COVID-19 surge also accelerated NYC Health + Hospitals’ plans of expanding its eConsult system, a tool that makes it easier for primary care providers and specialists to communicate about patients. During the surge, the public health system was able to add a total of 29 specialties to the existing list, now facilitating electronic referrals within a total of 203 specialty care areas. This expansion included over a dozen new pediatric specialty areas, in addition to urology, gastroenterology, and hematology/oncology. The proportion of referrals that were managed with an electronic eConsult electronically rose from 12 percent to 18 percent during the peak of the pandemic.
- Behavioral Health: While NYC Health + Hospitals clinics remained open for urgent mental health needs, Behavioral Health services were similarly converted to telehealth. Within two months NYC Health + Hospitals psychiatrists and therapists provided more than 30,000 behavioral health and addiction treatment phone and video visits. This major shift into telemedicine was enabled by policy changes from New York State Office of Mental Health (OMH) and Office of Addiction Services and Supports (OASAS).
- Coordinated Care: In addition to medical care, NYC Health + Hospitals transitioned its financial counseling workforce to televisits, providing essential support so that ability to pay would not be a barrier to care. Eligible patients could continue to receive health insurance guidance and enroll in programs like NYC Care telephonically. Social workers and the care coordination workforce also transitioned to providing essential patient outreach and support via telephone, helping ensure that patients’ social needs were met during this difficult time.
- Monitoring Patients After Discharge: NYC Health + Hospitals implemented a texting-based post-discharge symptom monitoring program through which patients would self-report symptoms daily. Any alarming results would trigger a physician callback, targeting this higher level of care to patients who needed it most. Text messages provided a low-cost, scalable, and patient-centered means of communication, allowing the public health system to direct its provider resources toward those patients most in need.
“Given what we know about how chronic diseases and healthcare disparities increase a person’s risk of succumbing to coronavirus, it was imperative for our public health system to maintain access for our nearly 500,000 clinic patients, many of whom are particularly vulnerable,” said Janine Knudsen, MD, Medical Director of Primary Care Transformation at NYC Health + Hospitals’ Office of Population Health. “We are committed to ensuring that all patients have the ability to access care safely from home, whether it be for routine appointments, renewing prescriptions, or social service needs.”
“Our prior investments in crucial technological infrastructure, such as a unified EMR system, an online patient-portal, and text-based communications helped us stay connected and provide New Yorkers the high-quality care they needed during a deadly pandemic,” said Jen Lau, Senior Director of Primary Care Transformation at NYC Health + Hospitals’ Office of Population Health. “Smart investments from the past, and a deep understanding of our patients’ needs and access, allowed our telehealth expansion to be all the more successful.”
“The ability to scale up and expand existing telehealth services to New Yorkers required an all-systems approach and collaboration,” said Hannah Jackson, MD MPH, Assistant Vice President and Chief of Staff for the Office of Ambulatory Care at NYC Health + Hospitals. “With more than half of our ambulatory care staff redeployed to inpatient services and public-facing COVID-19 testing, our clinics relied heavily on telehealth to maintain essential services for our patients and ensure that those with serious medical issues were getting care in a timely and safe way. Together, we were able to manage and balance the ever-changing demands of this unprecedented pandemic.”
Virtual tools also helped NYC Health + Hospitals mitigate the emotional toll of being isolated in the hospital during these challenging times. Using over 1,000 donated tablets, patients who were unable to receive visitors due to strict but necessary restrictions were able to connect with their loved ones through a newly implemented patient-family community program. NYC Health + Hospitals helped facilitate over 500 video calls a day to connect patients and their loved ones.
A patient survey that year revealed that over 65 percent of existing NYC Health + Hospitals patients were interested in telehealth, including 40 percent of respondents over the age of 65. In addition, the survey found 75 percent of respondents used their cell phones to access the internet, highlighting the need for mobile interventions.
NYC Health + Hospitals began building its system-wide telehealth strategy in 2017. A patient survey that year revealed that over 65 percent of existing NYC Health + Hospitals patients were interested in telehealth, including 40 percent of respondents over the age of 65. In addition, the survey found 75 percent of respondents used their cell phones to access the internet, highlighting the need for mobile interventions.
NYC Health + Hospitals is the largest public health care system in the nation serving more than a million New Yorkers annually in more than 70 patient care locations across the city’s five boroughs. A robust network of outpatient, neighborhood-based primary and specialty care centers anchors care coordination with the system’s trauma centers, nursing homes, post-acute care centers, home care agency, and MetroPlus health plan—all supported by 11 essential hospitals. Its diverse workforce of more than 42,000 employees is uniquely focused on empowering New Yorkers, without exception, to live the healthiest life possible. For more information, visit www.nychealthandhospitals.org
Become a Harlem Insider!
By submitting this form, you are consenting to receive marketing emails from: Harlem World Magazine, 2521 1/2 west 42nd street, Los Angeles, CA, 90008, https://www.harlemworldmagazine.com. You can revoke your consent to receive emails at any time by using the SafeUnsubscribe® link, found at the bottom of every email. Emails are serviced by Constant Contact